Welcome to Lesson 2 in this lesson-series on Post-Covid Syndrome. In this lesson, we will explore the Causes to Post-Covid Syndrome by examining four key contributing factors. Our goal is to help patients and other readers better understand the complexities of Post-Covid Syndrome, leading to more informed decisions, improved treatments, and optimal treatment results toward an improved qualify of life.
What are the Causes to Post-Covid Syndrome? #
Post-Covid Syndrome is a complex and multifaceted condition that affects a significant number of individuals who have recovered from the acute phase of COVID-19. The pathogenesis of Post-Covid Syndrome is not yet fully established, as it is still a relatively new condition that researchers are actively studying. However, in the integrative and holistic community of doctors and scientists, the following factors are agreed to be the causes to Post-Covid Syndrome:
1. Continuance of immune system dysregulation resulting in ongoing inflammatory conditions
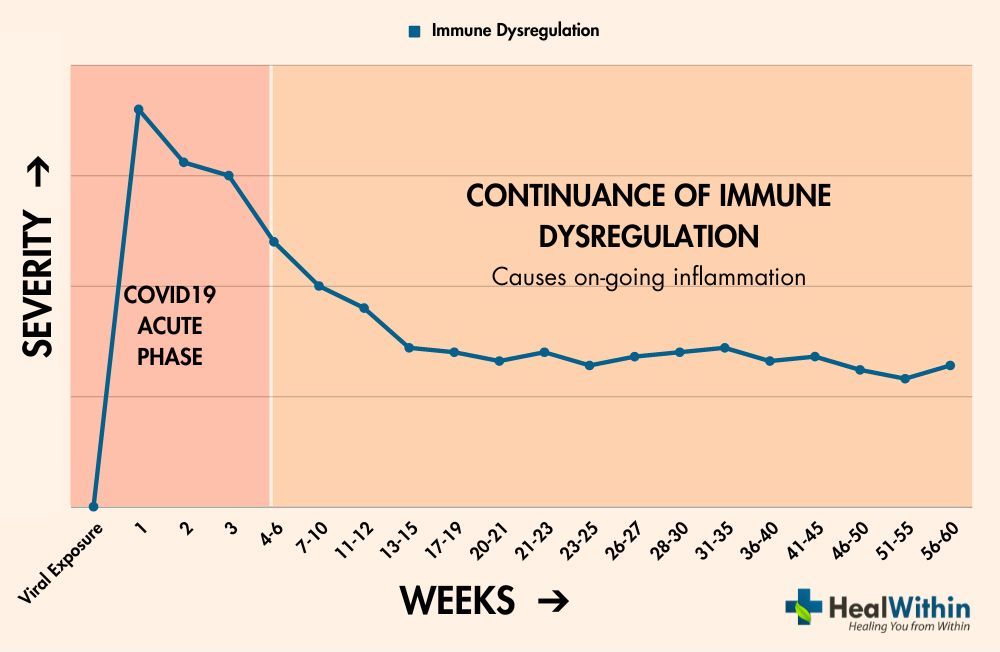
Immune system dysregulation refers to an imbalance or malfunction in the body’s immune response, which can lead to either an underactive or overactive immune reaction. Under normal circumstances, the immune system works to protect the body from harmful pathogens and maintain overall health. However, when dysregulation occurs, the immune system may fail to function optimally, potentially leading to chronic inflammation or an increased susceptibility to infections.
One of the primary factors contributing to the development of Post-Covid Syndrome is the continuance of immune system dysregulation, which leads to ongoing inflammatory conditions. In some individuals who have recovered from the acute phase of COVID-19, the immune system may remain imbalanced, causing a persistent inflammatory response that impacts various organs and tissues.
Cytokines and other immune mediators play a significant role in perpetuating inflammation. Cytokines are small proteins released by immune cells that help regulate the immune response. In some cases, an overproduction of pro-inflammatory cytokines, known as a cytokine storm, can occur, leading to widespread inflammation and tissue damage. This excessive inflammation can persist even after the virus has been cleared from the body, potentially contributing to the symptoms experienced by those with Post-Covid Syndrome.
Viral debris, which refers to remnants or debris of the virus, may also contribute to the continuance of immune system dysregulation. Some researchers believe that viral debris may persist in the body even after the acute infection has resolved. The presence of this debris could cause the immune system to remain active and continue producing inflammatory mediators, thereby perpetuating the inflammatory response. As a result, individuals with Post-Covid Syndrome may experience a range of symptoms associated with ongoing inflammation, such as fatigue, joint pain, and cognitive difficulties.
2. Exacerbation of inflammatory conditions associated with chronic diseases that existed prior to COVID-19
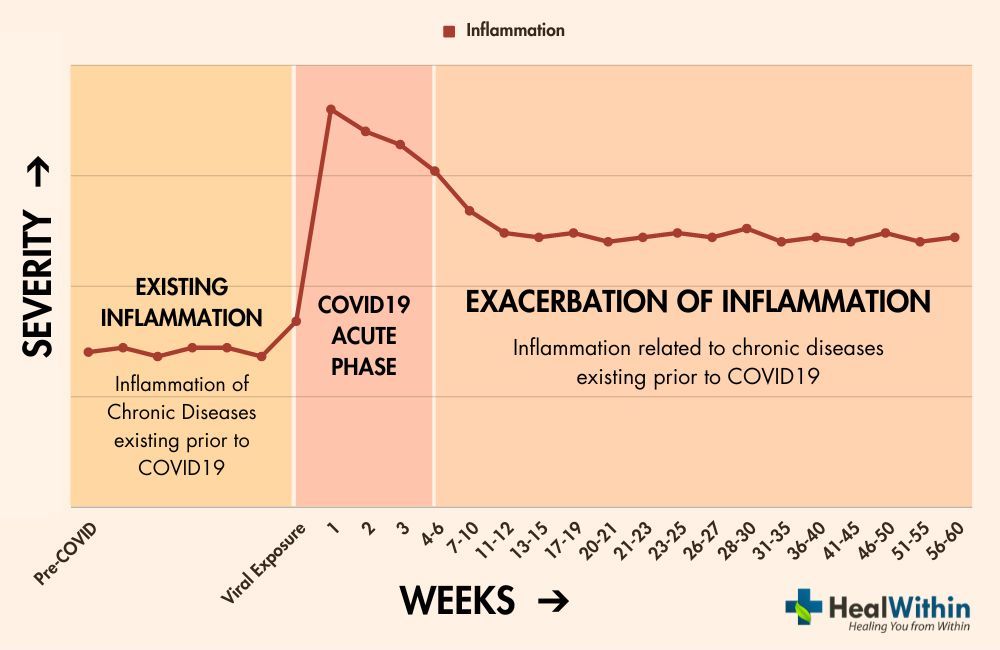
Another factor that may contribute to the development of Post-Covid Syndrome is the exacerbation of inflammatory conditions associated with chronic diseases that existed prior to the COVID-19 infection. Individuals with pre-existing chronic conditions, such as heart disease, diabetes, chronic respiratory diseases or even auto-immune conditions, may experience a more severe course of Post-Covid Syndrome due to the interplay between their underlying disease and the immune response to the virus.
In the case of heart disease, the inflammation triggered by the immune system’s response to COVID-19 may cause further damage to the cardiovascular system. This damage may include an increased risk of blood clots, myocardial injury, or worsening of pre-existing heart conditions. The pathophysiological mechanisms underlying this process involve the activation of immune cells and the release of inflammatory mediators that can directly or indirectly damage cardiac tissue.
For patients with diabetes, the immune response to COVID-19 may exacerbate existing inflammation related to high blood sugar levels. This inflammation can impair the normal function of blood vessels and other tissues, potentially worsening the complications associated with diabetes. The pathophysiological mechanisms in this case involve the impact of hyperglycemia on immune cell function, leading to an imbalanced response and increased inflammation.
Similarly, individuals with chronic respiratory diseases, such as asthma or chronic obstructive pulmonary disease (COPD), may experience worsening of their condition due to the inflammatory response associated with COVID-19. The immune system’s reaction to the virus can cause increased inflammation in the lungs, exacerbating existing respiratory conditions and potentially leading to more severe symptoms. The underlying pathophysiological mechanisms involve the activation of immune cells and the release of inflammatory mediators that contribute to airway inflammation and damage.
Auto-immune conditions, in which the immune system mistakenly attacks the body’s own tissues, can also be exacerbated by the immune response to COVID-19. In individuals with auto-immune disorders like rheumatoid arthritis or lupus, the immune system’s reaction to the virus may trigger a flare-up of their condition, leading to increased inflammation and worsening of symptoms. The pathophysiological mechanisms underlying this process involve the dysregulation of the immune system, which can be further impacted by the immune response to the virus.
In each of these cases, the underlying chronic disease may interact with the immune response to COVID-19, leading to an exacerbation of the existing inflammatory conditions prior to COVID-19 and potentially contributing to the development of Post-Covid Syndrome.
3. Exacerbation of silent inflammatory conditions that existed prior to COVID-19
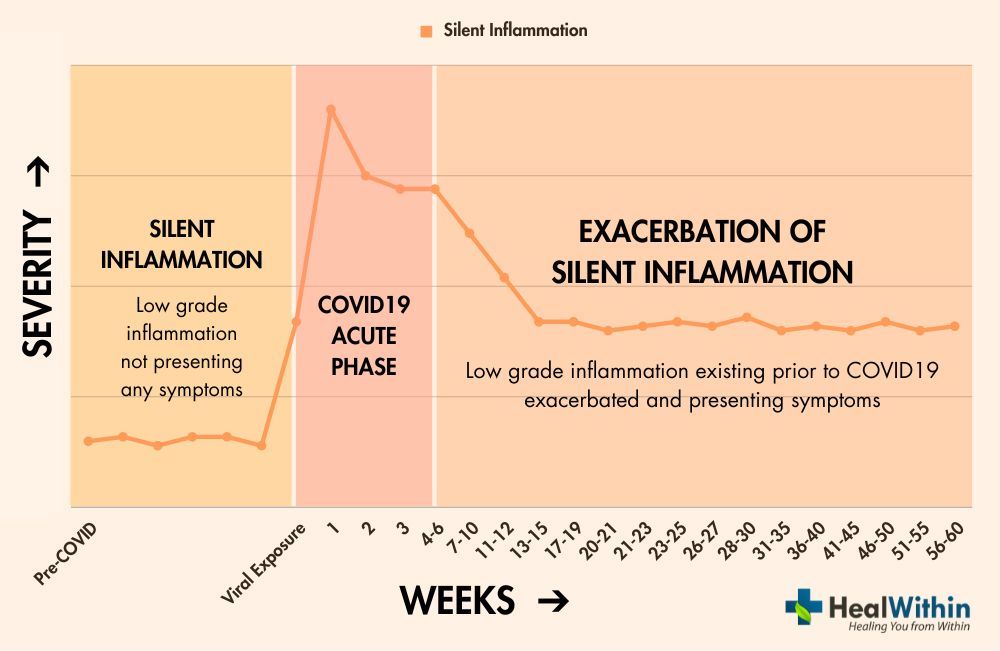
The development of Post-Covid Syndrome can also be influenced by the exacerbation of silent inflammatory conditions that existed before the COVID-19 infection. Silent inflammation refers to a low-grade, chronic inflammatory state that may not be immediately apparent or cause noticeable symptoms. These silent inflammatory conditions can include subclinical infections, low-grade autoimmune reactions, or underlying metabolic imbalances.
During the immune response to COVID-19, the immune system’s activation may inadvertently exacerbate these pre-existing silent inflammatory conditions. The release of inflammatory mediators and activation of immune cells can amplify the inflammation, potentially causing it to become more noticeable and symptomatic. This heightened inflammatory state may contribute to the development of Post-Covid Syndrome in some individuals.
For instance, individuals with subclinical infections, such as a low-grade bacterial infection, may experience a worsening of their condition as the immune system’s response to COVID-19 increases the overall inflammatory burden in the body. The pathophysiological mechanisms in this case involve the heightened immune response, which may exacerbate the inflammation associated with the underlying infection.
Similarly, individuals with low-grade autoimmune reactions or underlying metabolic imbalances may experience a worsening of their silent inflammatory conditions due to the immune system’s reaction to COVID-19. The immune response to the virus can further dysregulate the immune system and increase inflammation, thereby aggravating these pre-existing conditions and potentially leading to the development of Post-Covid Syndrome.
In summary, the exacerbation of silent inflammatory conditions that existed prior to COVID-19 can play a significant role in the pathogenesis of Post-Covid Syndrome. The immune system’s reaction to the virus may inadvertently worsen these pre-existing conditions, potentially contributing to the development of the syndrome and its associated symptoms.
4. Unresolved damage to organs that occurred during COVID-19 Acute Phase
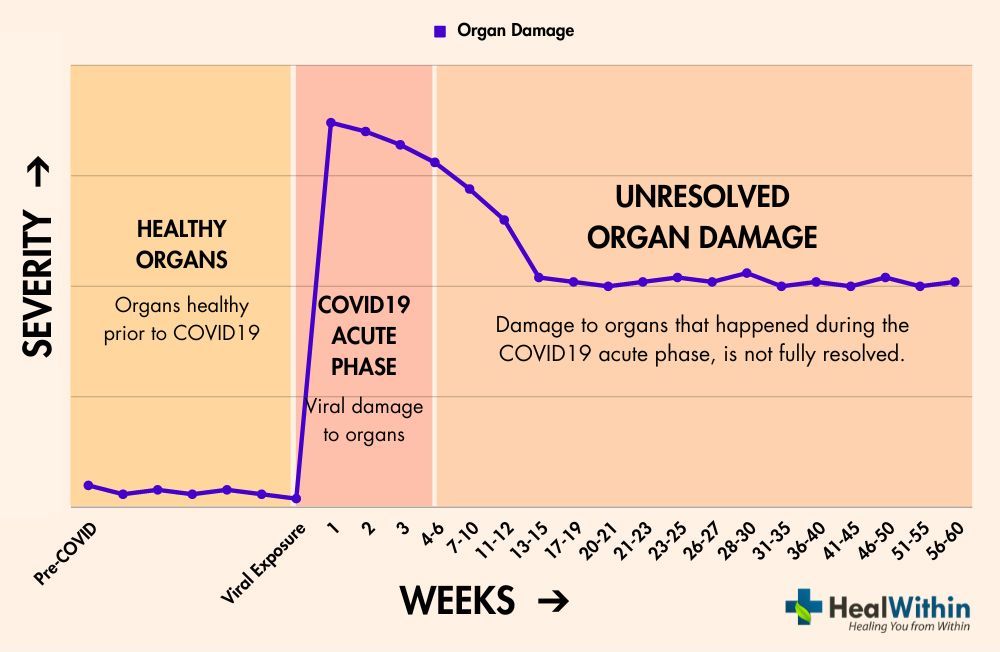
Unresolved damage to organs that occurred during the acute phase of SARS-CoV-2 viral infection can also contribute to the development of Post-Covid Syndrome. The virus has been shown to affect various organs and tissues throughout the body, including the lungs, heart, kidneys, and nervous system. In some cases, the damage caused by the virus may not be completely resolved during the recovery process, leaving lasting effects on the affected organs.
For example, in the case of lung damage, the virus can cause inflammation and injury to the lung tissue, leading to respiratory complications such as pneumonia. In some individuals, this damage may not be entirely resolved during the recovery process, potentially resulting in long-term respiratory symptoms such as shortness of breath or reduced lung function. The underlying pathophysiological mechanisms involve the persistent inflammation and scarring of lung tissue, which can impair the normal function of the respiratory system.
Similarly, the virus can cause damage to the heart, leading to conditions such as myocarditis or heart failure. If the damage to the heart tissue is not fully resolved during the recovery process, it may contribute to the development of Post-Covid Syndrome by causing ongoing cardiovascular symptoms such as palpitations, chest pain, or fatigue. The pathophysiological mechanisms in this case involve the lasting effects of inflammation and injury on the heart tissue, which can impair the normal function of the cardiovascular system.
Furthermore, damage to other organs, such as the kidneys or the nervous system, may also contribute to the development of Post-Covid Syndrome if not fully resolved. The pathophysiological mechanisms in these cases involve the lingering effects of inflammation, injury, or dysfunction on the affected organs, which can lead to a range of symptoms associated with Post-Covid Syndrome.
In summary, unresolved damage to organs that occurred during SARS-CoV-2 viral infection can play a significant role in the pathogenesis of Post-Covid Syndrome. The lingering effects of inflammation and injury on the affected organs may contribute to the development of the syndrome and its associated symptoms, even after the acute phase of the infection has resolved.
Summary and Conclusion #
Post-Covid Syndrome, is a complex condition that affects many individuals after recovering from the acute phase of COVID-19. The Causes to Post-Covid Syndrome can be attributed to these factors:
- Continuance of immune system dysregulation resulting in ongoing inflammatory conditions.
- Exacerbation of inflammatory conditions associated with chronic diseases that existed prior to Covid-19.
- Exacerbation of silent inflammatory conditions that existed prior to COVID-19.
- Unresolved damage to organs that occurred during SARS-CoV-2 viral infection.
Understanding the pathophysiology of Post-Covid Syndrome is crucial for patients and healthcare providers to manage and treat the condition effectively. We have discussed the detailed pathophysiological changes in various categories of COVID-19 cases, including patients with existing chronic diseases, patients that had organ damage during the acute phase, and patients with existing silent inflammation. By recognizing these factors and their effects on various organ systems, patients and healthcare providers can work together to develop individualized care plans and strategies to manage and alleviate the symptoms of Post-Covid Syndrome.
As we continue to learn more about Post-Covid Syndrome, it is essential to stay informed and updated on the latest research and advancements in the understanding and treatment of this condition. By doing so, we can better support those who are affected by Post-Covid Syndrome and help them on their journey towards recovery and improved quality of life.
























