Welcome to Lesson 3 in this lesson-series on Post-Covid Syndrome. In this lesson, we will dive deeper into the diagnostic process. We will explore why symptoms alone are not sufficient for diagnosing Post-Covid Syndrome and discuss the standard medical method for diagnosing this condition. Then, I will guide you through the comprehensive integrated and holistic diagnostic process, detailing the various methods and tests utilized to identify the underlying causes to Post-Covid Syndrome.
By the end of this lesson, you will understand the importance of a thorough, integrated, and holistic diagnostic approach for accurately identifying Post-Covid Syndrome.
What is the standard method in conventional medicine to diagnose Post-Covid Syndrome? #
As of the date of publishing this lesson, there is no established nor any clear-cut diagnostic protocol in Conventional Medicine (i.e., standard western medicine as per WHO) to diagnose Post-Covid Syndrome. Due to this absence of a universally accepted diagnostic standard, conventional medicine doctors often rely on general guidelines and/or general consensus to approximate a diagnosis of Post-Covid Syndrome.
In contrast, we, as integrated & holistic medical practitioners, have developed an approach to address this challenge by using an integrated & holistic diagnostic method to diagnose Post-Covid Syndrome, which we will discuss in the next section.
What is the Integrated & Holistic approach to diagnose Post-Covid Syndrome? #
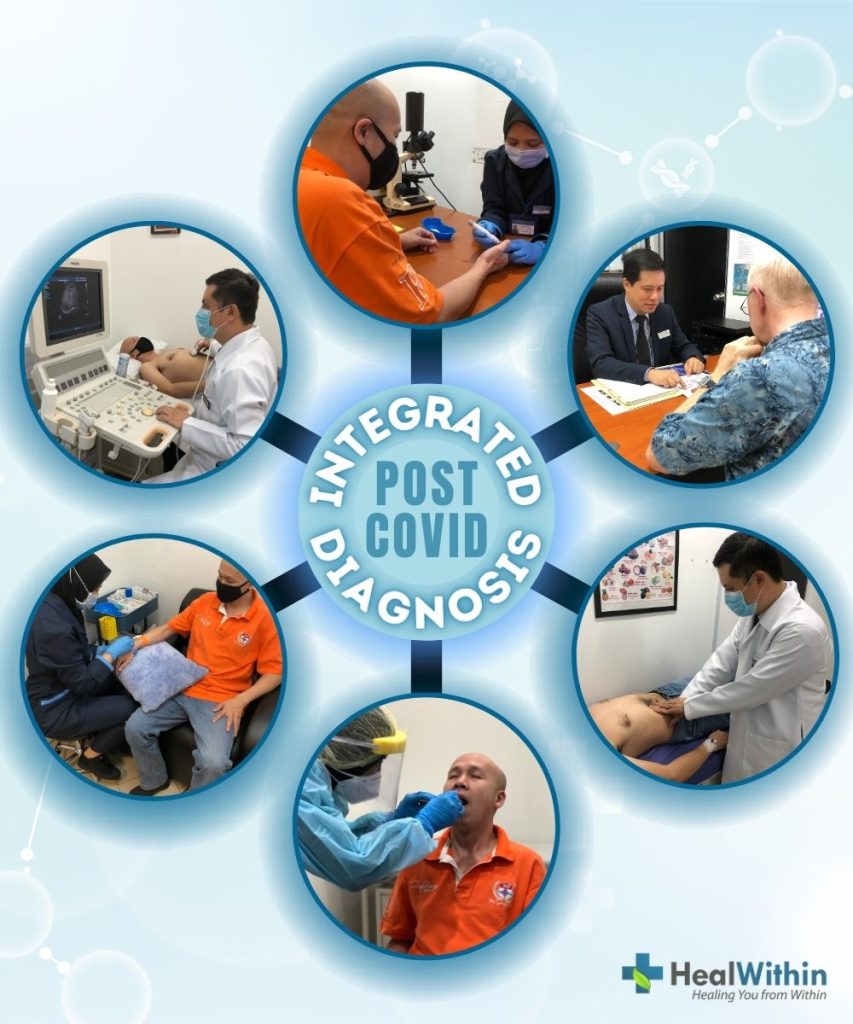
To better understand the integrated and holistic approach to diagnosing Post-Covid Syndrome, let’s first revisit the definition of Post-Covid Syndrome as explained in Lesson 1 of this series. Post-Covid Syndrome is a term used to describe a set of symptoms experienced by a person even after a SARS-CoV-2 viral infection has been treated (i.e., after COVID-19 is treated). These symptoms can be caused by one or more of the following underlying conditions: the continuance of immune system dysregulation triggered by the viral infection, exacerbation of inflammatory conditions associated with chronic diseases that existed prior to COVID-19, exacerbation of silent inflammatory conditions that existed prior to COVID-19, and/or unresolved organ damage that occurred during COVID-19.
The goal of the integrated and holistic approach is not to diagnose Post-Covid Syndrome itself, but rather to identify which of these underlying conditions are causing the symptoms associated with Post-Covid Syndrome. More importantly, this approach seeks to diagnose the root causes of these underlying conditions. An accurate diagnosis of Post-Covid Syndrome is crucial for providing targeted and effective treatment to patients. This comprehensive approach considers not only the physical aspects of the condition but also the mental and emotional factors that may contribute to the persistence of symptoms. In the following sections, we will discuss the process that integrated and holistic doctors use to diagnose the various aspects of Post-Covid Syndrome, focusing on immune system dysregulation, exacerbated inflammatory conditions, silent inflammatory conditions, and unresolved organ damage.
1. Medical history assessment

What it is:
Medical history assessment involves gathering detailed information about a patient’s past and present health conditions, including their experience with COVID-19. This assessment aims to understand the patient’s overall health background and identify any factors that could be contributing to the development or persistence of Post-Covid Syndrome.
Why it's done:
A thorough medical history assessment is essential for diagnosing Post-Covid Syndrome because it can provide valuable insights into the possible underlying conditions causing the symptoms. Additionally, understanding the patient’s medical history can help identify existing chronic diseases or silent inflammatory conditions that may have been exacerbated by COVID-19, or reveal previously undiagnosed conditions that could be contributing to the syndrome.
How it's done:
During a medical history assessment, the doctor will ask the patient a series of questions about their past and present health conditions, including questions about:
- Their experience with COVID-19, including the severity of the infection and any treatments received;
- Previous medical conditions, including any chronic diseases or inflammatory conditions;
- Previous silent inflammatory conditions;
- Family medical history, as certain conditions may have a genetic component;
- Medications and supplements currently being taken;
- Lifestyle factors, such as diet, exercise, stress levels, rest patterns, etc.
What specific indications suggest Post-Covid Syndrome:
Some indications from a patient’s medical history assessment, that may suggest Post-Covid Syndrome include:
- A history of severe or prolonged COVID-19 infection and possibility of unresolved organ damage that happened during the acute phase, which may increase the risk of developing Post-Covid Syndrome
- The presence of chronic diseases or inflammatory conditions that may have been exacerbated by COVID-19
- The presence of silent inflammatory conditions that may have been exacerbated by COVID-19
- A pattern of symptoms that align with the known symptoms of Post-Covid Syndrome, persisting or appearing after the acute phase of COVID-19 has resolved
- A lack of improvement or worsening of symptoms despite receiving treatment for other diagnosed conditions, suggesting that another underlying issue may be contributing to the patient’s symptoms
2. Clinical examination
What it is:
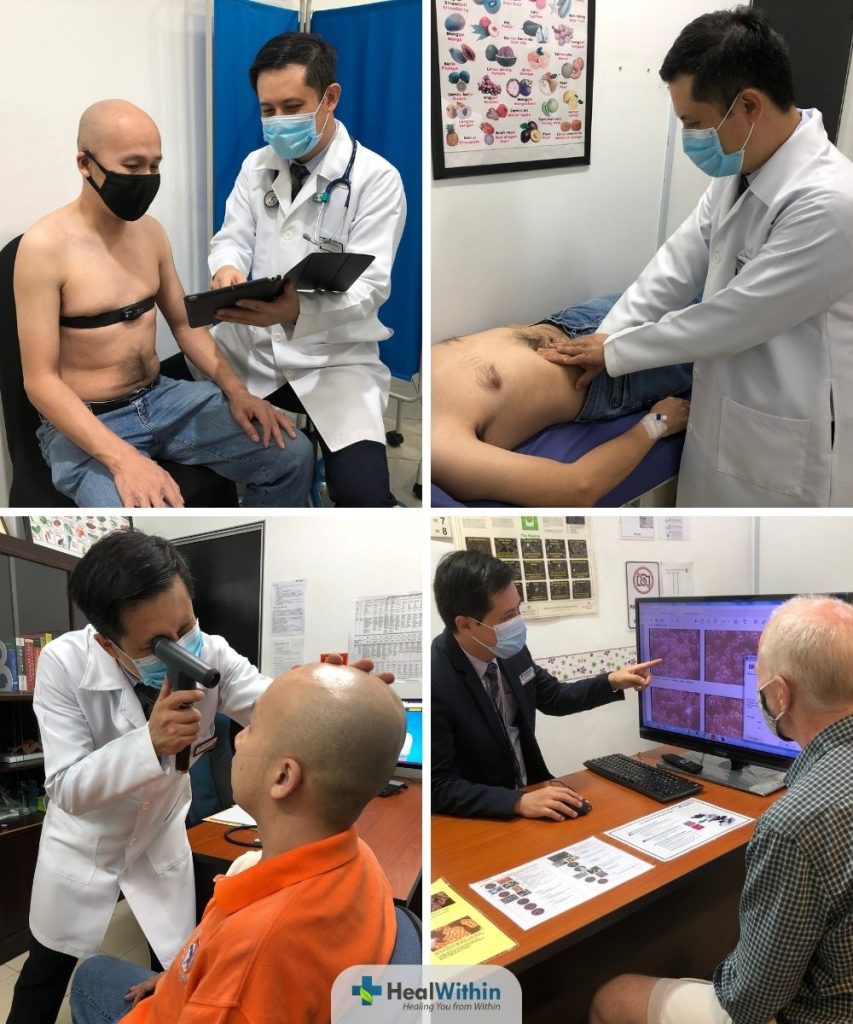
A clinical examination is a comprehensive physical examination conducted by a healthcare professional to assess a patient’s overall health and identify any signs or symptoms that may be indicative of Post-Covid Syndrome or other health conditions.
Why it's done:
Clinical examinations are essential for diagnosing Post-Covid Syndrome as they can help detect physical manifestations of the syndrome and provide crucial information about the patient’s current health status. The examination can also help rule out other health conditions that may present similar symptoms, ensuring that the diagnosis is accurate.
How it's done:
During a clinical examination, the healthcare professional will perform a thorough evaluation of the patient’s physical health, focusing on the areas where symptoms have been reported. This may include:
- Assessing vital signs such as blood pressure, heart rate, respiratory rate, and temperature
- Examining the skin for rashes, lesions, or other abnormalities
- Listening to the patient’s heart and lungs using a stethoscope to identify any abnormal sounds or rhythms
- Evaluating the patient’s neurological function, including assessing cognitive function, reflexes, and coordination
- Palpating the abdomen to check for tenderness, bloating, or masses
- Assessing muscle strength and joint mobility
- Any other examinations deemed necessary based on the patient’s medical history and reported symptoms
What specific indications suggest Post-Covid Syndrome:
Certain findings during a clinical examination may suggest Post-Covid Syndrome, including:
- Persistent tachycardia (elevated heart rate) or irregular heart rhythms, which can be indicative of ongoing cardiac issues related to the syndrome
- Abnormal lung sounds, such as crackles or wheezing, suggesting unresolved respiratory complications
- Cognitive difficulties, such as memory or concentration problems, which are commonly reported in Post-Covid Syndrome patients
- Signs of inflammation or tenderness in the joints or muscles, indicating a possible underlying inflammatory condition
- Any other physical signs that align with the known symptoms of Post-Covid Syndrome and cannot be explained by another diagnosed condition
3. RT-PCR test:
What it is:
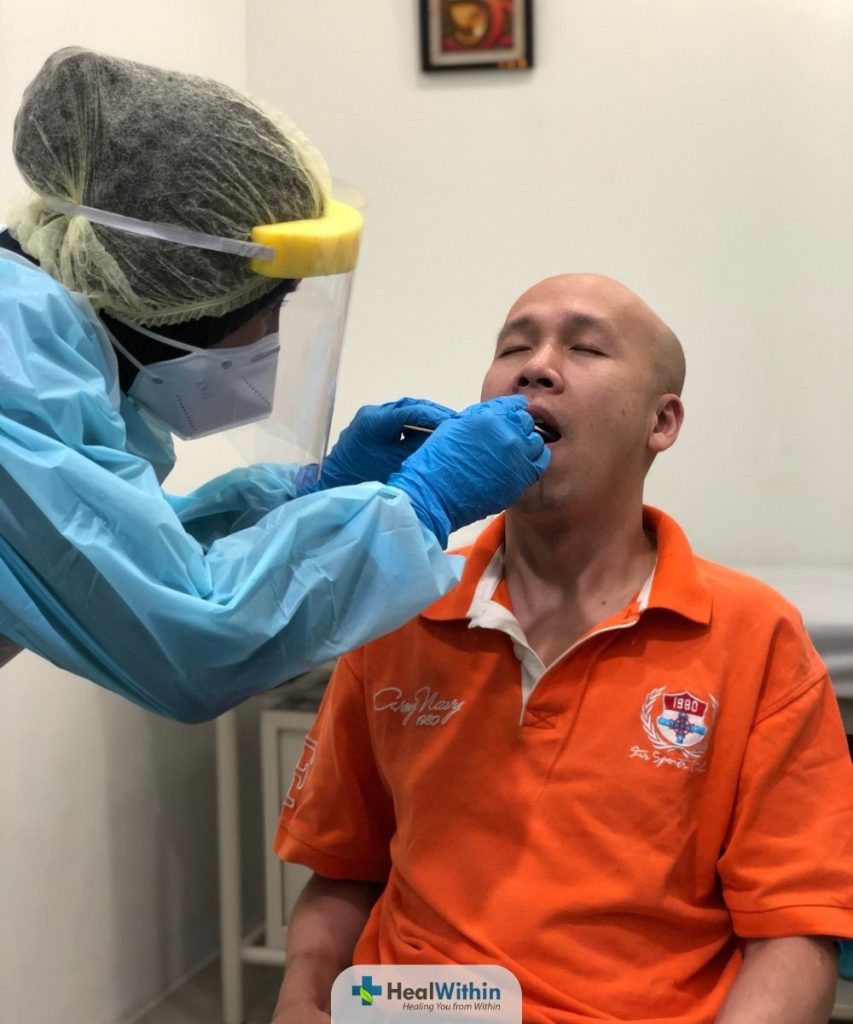
The RT-PCR (Reverse Transcription-Polymerase Chain Reaction) test is a diagnostic tool used to detect the presence of SARS-CoV-2, the virus responsible for COVID-19, in a patient’s respiratory samples. This test is highly sensitive and specific for detecting viral genetic material, making it a reliable method for diagnosing active COVID-19 infections.
Why it's done:
The RT-PCR test is performed to assess whether a patient with symptoms similar to Post-Covid Syndrome has an active SARS-CoV-2 infection. This test helps to differentiate between ongoing COVID-19 infection and Post-Covid Syndrome, as the symptoms of both conditions can be similar. Identifying whether a patient has an active infection is important for determining the appropriate course of treatment and managing potential complications.
How it's done:
The RT-PCR test is typically performed using a respiratory sample collected from the patient, such as a nasopharyngeal or oropharyngeal swab. The sample is then analyzed in a laboratory using specialized equipment and techniques to detect the presence of the virus’s genetic material. The test results are usually available within a few hours to a couple of days, depending on laboratory capacity and testing demand.
What specific indications suggest Post-Covid Syndrome:
A negative RT-PCR test result, indicating the absence of an active SARS-CoV-2 infection, can help support the diagnosis of Post-Covid Syndrome in patients experiencing persistent or new symptoms after recovering from COVID-19. However, it’s important to note that a negative RT-PCR test alone is not enough to diagnose Post-Covid Syndrome, as other diagnostic methods and assessments should be used in conjunction to establish a comprehensive understanding of the patient’s condition.
4. IgG Antibody test:
What it is:
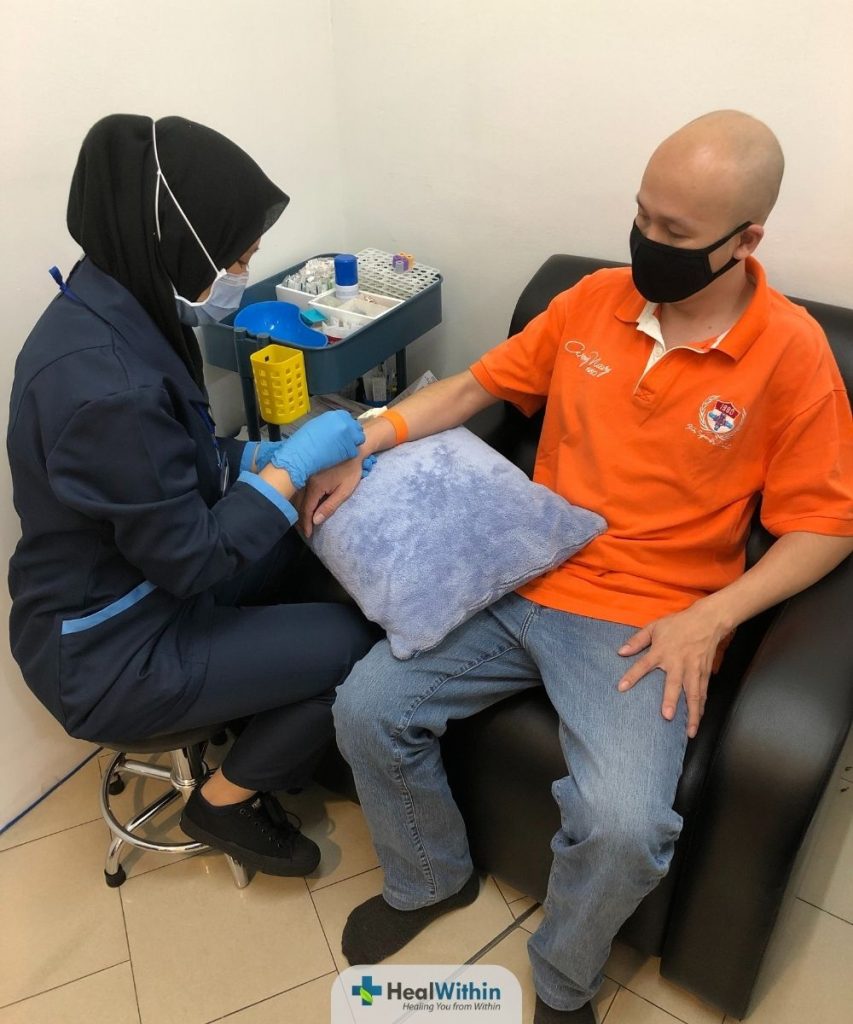
The IgG (Immunoglobulin G) antibody test is a blood test used to detect the presence of antibodies specific to the SARS-CoV-2 virus. IgG antibodies are produced by the immune system in response to an infection and typically indicate a past exposure to the virus. These antibodies usually develop within a few weeks following the infection and can persist for months or even years.
Why it's done:
The IgG antibody test is performed to determine whether a patient has been previously exposed to the SARS-CoV-2 virus and has mounted an immune response. This information can be valuable for diagnosing Post-Covid Syndrome, as it helps to confirm that the patient had a prior COVID-19 infection. Moreover, it can provide insights into the patient’s immune system function and help guide treatment decisions.
How it's done:
The IgG antibody test involves collecting a blood sample from the patient, which is then analyzed in a laboratory for the presence of SARS-CoV-2-specific IgG antibodies. The test results are generally available within a few days to a week, depending on laboratory capacity and testing demand.
What specific indications suggest Post-Covid Syndrome:
A positive IgG antibody test result, indicating past exposure to the SARS-CoV-2 virus and subsequent immune response, can support the diagnosis of Post-Covid Syndrome in patients experiencing persistent or new symptoms after recovering from COVID-19. However, it’s important to note that a positive IgG test alone is not sufficient to diagnose Post-Covid Syndrome, as other diagnostic methods and assessments should be used in conjunction to establish a comprehensive understanding of the patient’s condition.
5. Immune system dysregulation tests:
What it is:
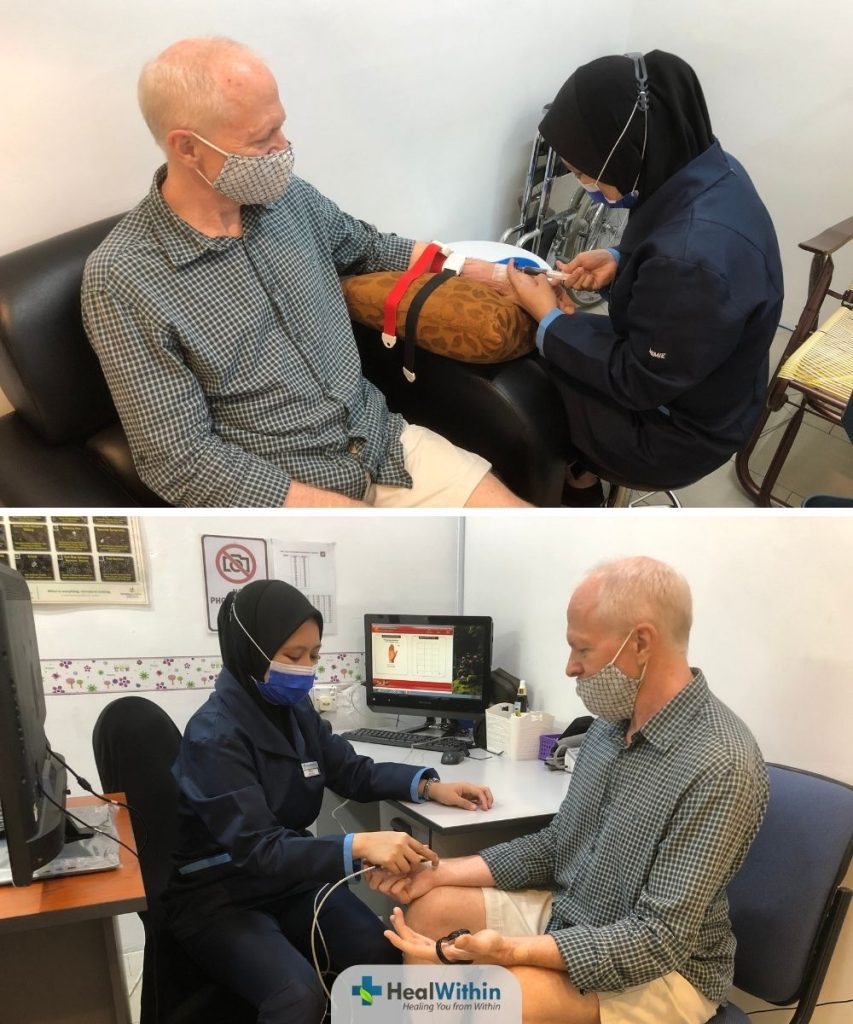
Immune system dysregulation refers to an imbalance in the body’s immune response, where the immune system either overreacts or underreacts to a threat, leading to chronic inflammation or increased susceptibility to infections. Immune system dysregulation tests are a series of tests designed to evaluate the immune system’s function and detect potential imbalances that could contribute to Post-Covid Syndrome.
Why it's done:
These tests are performed to assess whether immune system dysregulation could be an underlying cause of a patient’s Post-Covid Syndrome symptoms. Identifying immune system imbalances can help guide targeted treatment strategies aimed at restoring proper immune function and alleviating symptoms associated with Post-Covid Syndrome.
How it's done:
Immune system dysregulation tests typically involve a combination of blood tests and other diagnostic procedures to assess various aspects of the immune system’s function. Some common tests include:
- Complete blood count (CBC) with differential: This test evaluates the levels of different types of blood cells, including white blood cells, which play a crucial role in the immune system.
- Cytokine panel: This test measures the levels of specific proteins called cytokines, which are involved in immune system signaling and can contribute to inflammation when dysregulated.
- Immunoglobulin levels: This test measures the levels of immunoglobulins (antibodies) in the blood, which can help assess the immune system’s ability to respond to infections and other threats.
- Lymphocyte subset analysis: This test evaluates the levels and proportions of different types of lymphocytes (a type of white blood cell) involved in the immune response.
- Flow cytometry for immune cell analysis: This test uses a specialized technique to assess the presence, distribution, and function of various immune cells, providing a comprehensive overview of the immune system’s status.
What specific indications suggest Post-Covid Syndrome:
Indications of immune system dysregulation that may suggest Post-Covid Syndrome include abnormal results in one or more of the tests mentioned above. For example, altered cytokine levels, imbalanced lymphocyte subsets, abnormal immunoglobulin levels, or changes in immune cell populations detected by flow cytometry may indicate immune system dysfunction contributing to Post-Covid Syndrome symptoms. It’s essential to interpret these test results in conjunction with other diagnostic assessments and the patient’s medical history to establish a comprehensive understanding of the patient’s condition.
6. Blood Inflammatory Markers tests:
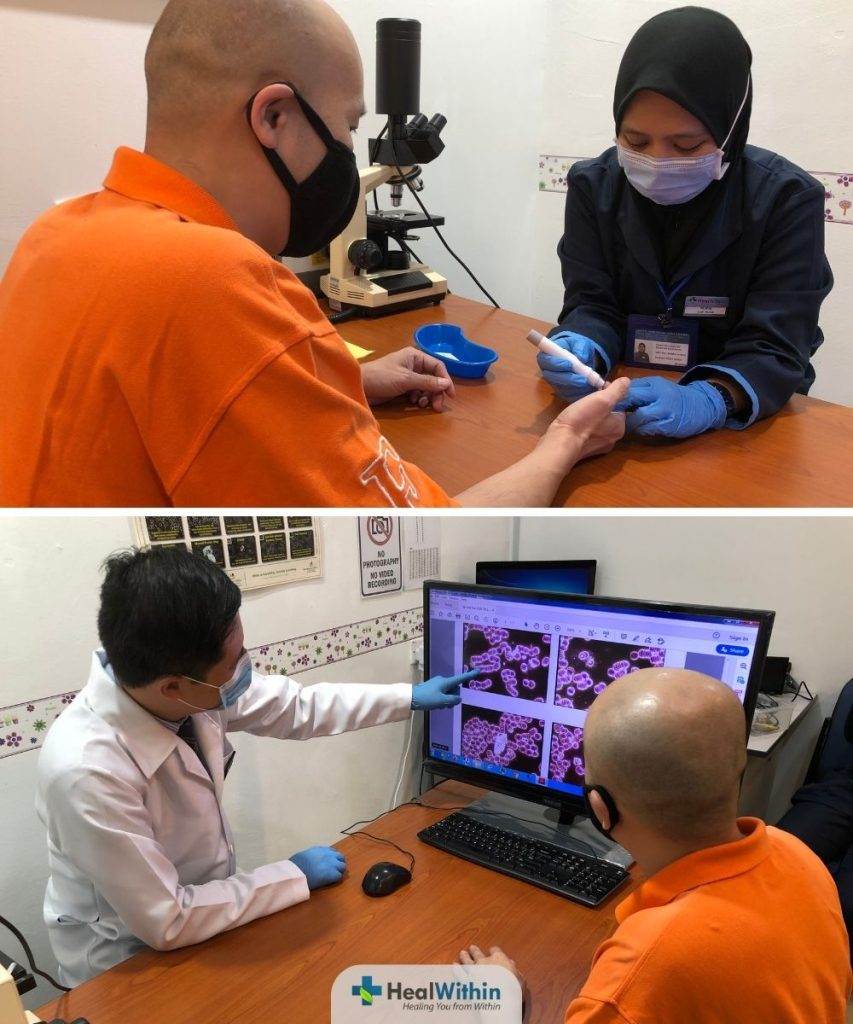
What it is:
Blood inflammatory markers tests are a set of tests that measure the levels of specific proteins in the blood, which can indicate the presence of inflammation in the body. These tests help identify any ongoing inflammation that could be contributing to Post-Covid Syndrome symptoms.
Why it's done:
These tests are performed to assess whether there is ongoing inflammation in the body, which could be caused by immune system dysregulation, exacerbated inflammatory conditions, or unresolved organ damage. Identifying the presence of inflammation can help guide treatment strategies aimed at reducing inflammation and alleviating symptoms associated with Post-Covid Syndrome.
How it's done:
Blood inflammatory markers tests typically involve taking a blood sample from the patient, which is then analyzed in a laboratory to measure the levels of specific proteins that indicate inflammation. Some common inflammatory markers tested include:
- C-reactive protein (CRP): An acute-phase protein that increases in the blood in response to inflammation.
- Erythrocyte sedimentation rate (ESR): A test that measures how quickly red blood cells settle at the bottom of a test tube, with an increased rate indicating inflammation.
- Interleukin-6 (IL-6): A pro-inflammatory cytokine that plays a role in the immune response and can contribute to inflammation when dysregulated.
- Tumor necrosis factor-alpha (TNF-alpha): A pro-inflammatory cytokine involved in the regulation of the immune system and inflammation.
What specific indications suggest Post-Covid Syndrome:
Elevated levels of one or more inflammatory markers in the blood may suggest ongoing inflammation in the body, which could be contributing to Post-Covid Syndrome symptoms. It’s essential to interpret these test results in conjunction with other diagnostic assessments and the patient’s medical history to establish a comprehensive understanding of the patient’s condition and determine the most appropriate treatment approach.
7. Imaging tests (CT-scans, X-ray, etc.):
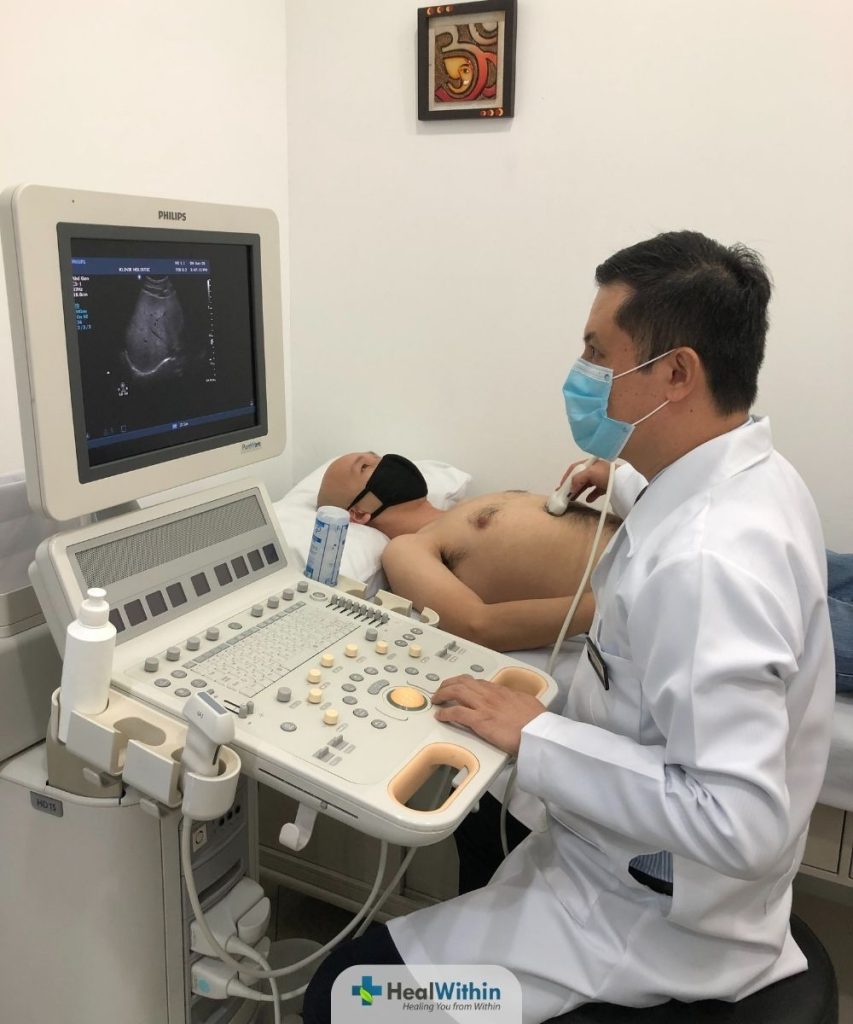
What it is:
Imaging tests, such as computed tomography (CT) scans, X-rays, and magnetic resonance imaging (MRI), are non-invasive diagnostic procedures used to visualize the internal structures of the body. These tests can help identify any unresolved organ damage that occurred during the acute phase of COVID-19, which may contribute to the persistence of Post-Covid Syndrome symptoms.
Why it's done:
Imaging tests are performed to assess potential organ damage that could be causing ongoing symptoms in patients with Post-Covid Syndrome. Unresolved organ damage can result from the acute phase of COVID-19 and may not have fully healed, leading to persistent symptoms and complications.
How it's done:
Imaging tests are performed by specialized medical professionals using advanced equipment. Some common imaging tests that may be used to assess unresolved organ damage in patients with Post-Covid Syndrome include:
- CT scan: A type of imaging that uses multiple X-ray images taken from different angles to create detailed cross-sectional images of the body. CT scans can be used to assess damage to the lungs, heart, or other organs.
- X-ray: A type of imaging that uses ionizing radiation to create images of the internal structures of the body. Chest X-rays are commonly used to evaluate lung damage caused by COVID-19.
- MRI: A type of imaging that uses a powerful magnet and radio waves to create detailed images of the body’s internal structures. MRI scans can be used to assess damage to the brain, heart, or other soft tissues.
What specific indications suggest Post-Covid Syndrome:
Imaging tests that reveal unresolved organ damage or abnormalities associated with the acute phase of COVID-19 can help confirm a diagnosis of Post-Covid Syndrome. Identifying such damage can guide treatment strategies to address the specific organ or tissue involved, thereby alleviating symptoms and improving the patient’s overall health. As with other diagnostic tests, it’s crucial to interpret imaging results in conjunction with the patient’s medical history and other diagnostic assessments for a comprehensive understanding of the patient’s condition.
Summary and Conclusion #
In conclusion, in this lesson I highlighted the importance of not relying solely on symptoms for diagnosing Post-Covid Syndrome due to their similarities with other chronic diseases. We also discussed the lack of a standard diagnostic protocol in conventional medicine and the importance to use of an integrated and holistic approach for diagnosing Post-Covid Syndrome.
The integrated and holistic diagnostic process, which involves a combination of medical history assessment, clinical examination, RT-PCR test, IgG antibody test, immune system dysregulation tests, blood inflammatory markers tests, and imaging tests for unresolved organ damage. It’s crucial to analyze the results of all tests holistically, as relying on a single test result may lead to an inaccurate diagnosis.
Addressing the underlying conditions causing Post-Covid Syndrome symptoms, such as immune system dysregulation, exacerbated inflammatory conditions, silent inflammatory conditions, and unresolved organ damage, is essential for effective treatment.
























